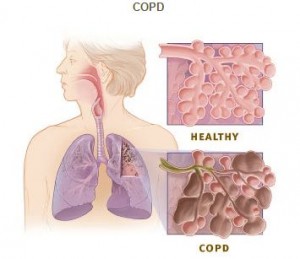
COPD is a chronic inflammatory lung disease that commonly affects both men and women worldwide. In patients with COPD, the airways may narrow due to a number of factors and processes, including abnormalities in the airways. There are two types of COPD — emphysema and chronic bronchitis. Emphysema affects the lungs’ alveoli (air sacs) and the walls between them; the air sacs get damaged and lose their elasticity. In chronic bronchitis, the lining of the airways is constantly inflamed — which causes it to swell and produce excess mucus.
Let’s take a look at some of the factors that can cause COPD:
In the early stage, patients may be asymptomatic (no symptoms) or present with mild symptoms. However, with the progression of the disease, the symptoms become severe. Some of the common symptoms include:
There are several tools that may be used to diagnose the condition:
Based on the results of these investigations, the doctor will diagnose the condition and start the appropriate COPD treatment.
COPD is typically managed according to the Global Initiative for Obstructive Lung Disease (GOLD) guidelines. The GOLD guidelines are used to classify COPD severity and provide recommendations for first-line treatment. Medications such as bronchodilators, oral steroids, inhaled steroids, combination inhalers, and antibiotics may be prescribed. The doctor may advise on steps such as smoking cessation and vaccination. Treatment may vary depending on the patient, symptoms, stage (early or advanced), severity, and compliance.
If a patient progresses rapidly from a stable condition to a severe one, it is referred to as a COPD exacerbation or flare-up. Exacerbations can last for days or even weeks. The two most common triggers for an exacerbation are respiratory tract infections, such as pneumonia and air pollution. There are some warning signs that may indicate a flare-up: more coughing, changes in the mucus (colour, thickness, and amount), and breathing difficulties.
Patients must seek immediate medical attention if the following occurs:
Patients may be referred to a pulmonologist for a severe and persistent cough lasting more than three weeks and/or any of the following symptoms:
The pulmonologist will take a detailed medical history and physical examination at the first visit and may order investigations to diagnose and manage the condition. The patient should bring any records of blood work and imaging to be assessed by the pulmonologist. In addition, it is wise to be prepared with any questions or doubts so that these can be clarified at the clinic.
Lung specialist A/Prof Philip Eng, who practises at Philip Eng Respiratory & Medical Clinic, specialises in respiratory and critical care management with a focus on evidence-based medicine and patient care. If you suspect you have a respiratory condition, get in touch with the clinic for more information or to book an appointment.